The Lip Tie/Tongue Tie Challenge
To help parents understand a bit more about how tongue and lip ties can affect breastfeeding, over the next few weeks we will be featuring stories from moms whose babies experienced these challenges. We would like to extend a HUGE thank you to the brave mamas who submitted their stories for our blog! We know you went through a ton of challenges and we are so appreciative that you were willing to share your stories! If you have a story you would like to share on our blog, please send it to robinkaplan@sdbfc.com.
For more information about tongue and lip ties and how they can affect breastfeeding, please see our article: Does Your Baby Have a Tongue or Lip Tie?
_____
Written by Julie Sanders
My issues with breastfeeding my daughter started pretty much as soon as we left the hospital. I started experiencing a lot of pain in my nipples. Not just while she was nursing, but all the time. I was told it was normal for her to nurse 8-10 times a day, but my daughter was nursing 20+ times a day. Essentially, she was constantly nursing, with maybe a 10-20 minute break between sessions. I found that since any side-lying, cradled position was extremely painful, only the football hold position worked for me. I went to a breastfeeding support group her second week, and I learned that my daughter was chomping my nipples while she nursed, and that’s why they were in constant pain. Nipples are supposed to come out of a baby’s mouth just as round as when they went in, but mine were shaped like a football after a nursing session. No wonder! Someone suggested I try nursing her lying down because she was perhaps trying to stem a strong flow of milk into her mouth, but that didn’t help. On top of it all, I also got a clogged duct, which was painful and scary. I was in such excruciating pain I would cry when my daughter wanted to nurse because I just wanted a break for my poor nipples to heal. I didn’t know why it was so hard or what was wrong. The only thing that got me through this period were gel pads. The moist, cold combination was wonderfully soothing.
To help parents understand a bit more about how tongue and lip ties can affect breastfeeding, over the next few weeks we will be featuring stories from moms whose babies experienced these challenges. We would like to extend a HUGE thank you to the brave mamas who submitted their stories for our blog! We know you went through a ton of challenges and we are so appreciative that you were willing to share your stories! If you have a story you would like to share on our blog, please send it to robinkaplan@sdbfc.com.
For more information about tongue and lip ties and how they can affect breastfeeding, please see our article: Does Your Baby Have a Tongue or Lip Tie?
_____
Written by Julie Sanders
My issues with breastfeeding my daughter started pretty much as soon as we left the hospital. I started experiencing a lot of pain in my nipples. Not just while she was nursing, but all the time. I was told it was normal for her to nurse 8-10 times a day, but my daughter was nursing 20+ times a day. Essentially, she was constantly nursing, with maybe a 10-20 minute break between sessions. I found that since any side-lying, cradled position was extremely painful, only the football hold position worked for me. I went to a breastfeeding support group her second week, and I learned that my daughter was chomping my nipples while she nursed, and that’s why they were in constant pain. Nipples are supposed to come out of a baby’s mouth just as round as when they went in, but mine were shaped like a football after a nursing session. No wonder! Someone suggested I try nursing her lying down because she was perhaps trying to stem a strong flow of milk into her mouth, but that didn’t help. On top of it all, I also got a clogged duct, which was painful and scary. I was in such excruciating pain I would cry when my daughter wanted to nurse because I just wanted a break for my poor nipples to heal. I didn’t know why it was so hard or what was wrong. The only thing that got me through this period were gel pads. The moist, cold combination was wonderfully soothing.
When my doula came over for our postpartum visit, she checked my daughter’s latch and suggested that we have her evaluated for a tongue tie. She said it didn’t look like her tongue reached far enough forward in her mouth (past the gums). We had never heard of a tongue tie before. She explained it is a very common, simple procedure our pediatrician could perform to snip the underside of her tongue to allow for greater mobility. I rejected the idea at first. The idea that my daughter wasn’t born with her mouth properly equipped to handle breastfeeding seemed ridiculous to me. My daughter was perfect in every way! But later that week when she had a wellness checkup, we asked about the tongue tie. Our pediatrician said it looked like there was indeed a tongue tie, and he would revise it if we wanted him to. So he clipped the frenulum under her tongue. It was done with scissors while the nurse and my husband held her down. He gave her just a topical gel to numb the area, then had to do about 3-4 snips to cut what he deemed enough. She wailed like I had never heard before and cried real tears. I cried real tears too. It was scarring. I nursed her immediately afterwards to help stop the bleeding and she slowly calmed down. The bleeding stopped very soon and she seemed on the road to recovery. She had a little discomfort for the next day or two. I thought the nightmare was finally over. But it wasn’t. At first I noticed a relief in how she nursed, but it was very short lived. I found out at the breastfeeding support group the next week that there were exercises we were supposed to be doing to help my daughter learn to use the full range of motion of her tongue. The lactation consultant who runs the group emailed me a video with instructions. I did them several times a day, as suggested, but nothing changed.
At around three weeks we finally saw a lactation consultant. I wish I had seen her during week one! Within minutes of telling her our history and examining my daughter, she told us my daughter also had a lip tie, and explained that my daughter nursed constantly because she was only able to get enough milk to satiate her for a short time before she would get hungry again. I hated the idea that my daughter had another tie. My perfect baby was still perfect! But we followed the advice of the lactation consultant and went to a pediatric dentist in the San Bernadino area who uses a laser instead of scissors, a tool that was supposedly less traumatic on both patient and parent. The thought of driving 80 miles with a baby so young almost deterred us, but we decided to go for it.
The dentist had my husband lie down in the chair and hold my daughter face up on his tummy. Being held by dad was far less traumatic than being pinned to a table by strangers. She also got to wear adorable little sunglasses to protect her eyes from the laser. The dentist checked her out and said she did indeed have a lip tie, and he wanted to do another revision on her tongue to cut more of the frenulum. It literally a minute per tie, if even. He lasered, she cried, and before I could even get upset he was done. I nursed her immediately, just like before, and she calmed very quickly. They gave me exercises to do with her several times a day to help the range of motion for her mouth. Once again I left with the feeling of “It’s over. It’s finally over.” But it wasn’t.
The discomfort again only lasted a day or two, and seemed a little worse for her lip than her tongue. I did the exercises but she just kept chomping. Though with the new mobility of her tongue, her bottom gums were padded a bit, and the pain, while still painful, was much more bearable by comparison. By this point I had gone through so much, I was determined to make this work. My lactation consultant had told us “body work” might be required. After all, my daughter had used her mouth to nurse a certain way her whole life thus far and she was used to it. So we went to a craniosacral therapist. The therapist observed my daughter while she nursed and felt all around her head to examine how her muscles were moving. She massaged around her head and jaw for a bit, and then she told us my daughter’s jaw was very tight, and that’s why she wasn’t latching correctly, but that there wasn’t anything she could do to loosen it.
Next we tried a chiropractor. Chiropractic was another kind of body work my lactation consultant had suggested we may need. She recommended a few people who worked with babies in my area. Over the next two weeks I saw the chiropractor three times. She adjusted areas in my daughter’s upper spine and around her jaw to try and loosen it. Between the three appointments and our periodic massaging of her jaw, gradually at around six to seven weeks old, my daughter’s jaw loosened, she stopped chomping my nipples, and started sucking the way Mother Nature intended. It felt like an eternity, but she is now three months old and our time breastfeeding is easy, a lovely bonding experience and no longer something I dread. It’s easy and wonderful, and it was worth every minute we spent at appointments and every dollar we spent on doctors and specialists and consultants.
I learned a great deal during this trial. A good lactation consultant is invaluable. Ours not only identified our issue right away, but she had all the references to specialists we needed. We were not in a place where we could have researched and found someone to go to on our own. We trusted our lactation consultant, we went where she sent us, and we were never disappointed. Surrounding myself with people who supported my determination to exclusively breastfeed was also pivotal. Being a new mom is an emotional time with many ups and downs even when breastfeeding is going well. My mental state really ran the gambit, and having people to tell me it would get better and that I could do it helped me through my lowest moments. The friend who introduced me to gel pads is an absolute saint! And I learned how strong a person I am. Compared to this experience, labor was easy. I always referred to what we were going through as “a breastfeeding challenge” because a challenge is something you overcome, and usually leaves you stronger and better off than when you started.
Does Your Baby Have a Tongue or Lip Tie?
Painful, cracked, compressed-after-breastfeeding nipples. Baby not gaining weight well. Constant breastfeeding sessions that seem to take over an hour. Excessive baby fussiness and gas. These are some of the many signs that your child may have a tongue and/or lip tie. So, what is a tongue and lip tie and how do they affect breastfeeding? What are ways to fix them and improve breastfeeding?
With several fantastic articles already written on this subject, we are going to give brief answers to these questions and link to our favorite comprehensive resources. Also, over the next month, we will be sharing stories from breastfeeding mothers whose babies had tongue and/or lip ties.
Painful, cracked, compressed-after-breastfeeding nipples. Baby not gaining weight well. Constant breastfeeding sessions that seem to take over an hour. Excessive baby fussiness and gas. These are some of the many signs that your child may have a tongue and/or lip tie. So, what is a tongue and lip tie and how do they affect breastfeeding? What are ways to fix them and improve breastfeeding?
With several fantastic articles already written on this subject, we are going to give brief answers to these questions and link to our favorite comprehensive resources. Also, over the next month, we will be sharing stories from breastfeeding mothers whose babies had tongue and/or lip ties.
What is a tongue tie and lip tie?
There are pieces of connective membranes under the tongue and behind the upper lip called frenula. Everyone has a lingual (tongue) frenulum and a labial (lip) frenulum, which means that if your baby has one, it doesn’t automatically mean that you are going to have breastfeeding challenges. It’s how the tongue and upper lip function that determine if the frenula are causing a problem.
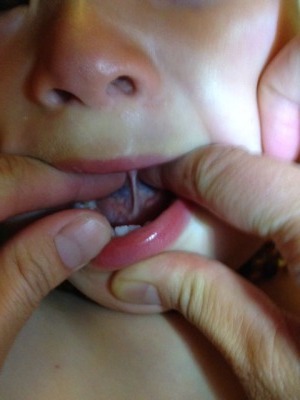
Tongue tie
Upper lip tie
How do tongue and lip ties cause breastfeeding challenges?
When the frenula are tight, they act like rubber bands, tethering down the tongue to the base of the mouth or the upper lip close to the upper gumline. This makes it difficult to move the tongue in an effective manner or flange the upper lip out. When the tongue doesn’t have full range of motion, it can cause all sorts of issues. Some moms’ nipples will be compressed, causing pain and ineffective milk extraction. Some babies will become very tired and fatigued while breastfeeding, having to work extra hard to compensate for the lack of range of motion in their tongues. This can turn into ineffective, long feedings and slow weight gain for babies. Other babies gain weight perfectly fine, but have tons of gas and excessive fussy periods because they are taking in so much air while breastfeeding due to the inability to push the milk back in a wavelike motion. Babies with tongue ties or significant lip ties often continually fall off the breast, as they are unable to form a good seal and suction. Other babies have such difficulty latching on to the breast that they refuse to breastfeed altogether.
Here are two articles that describe how tongue and lip ties can affect breastfeeding:
A Breastfeeding Mom’s Symptoms are as Important as Baby’s
Baby’s Weight Gain is Not the Only Marker of Successful Breastfeeding
Why didn’t my healthcare provider mention this to me?
Most health care providers have not been trained to assess and diagnose tongue or lip ties. Again, it is how the tongue and lip function (or not function) that cause the breastfeeding challenges. Most health care providers have not been trained to complete suck assessments on infants, therefore they cannot accurately assess what the tongue is doing while feeding. The best person to assess for a tongue or lip tie is a trained IBCLC (International Board Certified Lactation Consultant).
Who can treat my child’s tongue and/or lip tie and what are my options?
The best person to diagnose and treat a tongue or lip tie is a trained dentist, ENT (Ear, Nose, and Throat surgeon), oral surgeon, naturopath, pediatrician, or other medical professional trained to do minor surgery. Make sure to do your research, as not all professionals that revise tongue and lip ties know how to release them effectively. If the professional doesn’t do the revision procedure effectively and completely, then it will not fix the breastfeeding challenges completely and your baby may have to have the procedure again.
In most cases, the tongue or lip tie revision is done at an office visit. Some practitioners will numb the area before the procedure, although it isn’t necessary. Some practitioners, such as ENTs and pediatricians, may use blunt-edged scissors to snip the tight frenulum. Others, such as dentists, may use laser for the revision procedure.
Are there any negatives to having the tongue or lip tie revised?
There is very little risk for having your baby’s tongue or lip tie revised. Most parents comment after the procedure that their only regret is that they didn’t do it sooner, as it improved their breastfeeding challenges tremendously. Some babies may be a little fussy after the procedure, but most will settle with some extra cuddles. Some parents find that a little infant tylenol or homeopathy can help relieve pain (but always check with your healthcare provider for appropriate dosing.)
How can I keep the frenulum from scarring down after the procedure?
It is very important that parents do suck and stretching exercises after the procedure to prevent scarring down. My colleague, Melissa Cole, IBCLC, created this quick and easy video for suck exercises after tongue tie revisions: http://vimeo.com/55658345. She recommends doing these a few times a day, during baby’s quiet alert time, to retrain baby’s tongue to suck effectively and to prevent scarring down. A local dentist recommends bending baby’s upper lip up to his/her nose after an upper lip tie release to prevent scarring down.
Will my breastfeeding challenges resolve immediately after the procedure?
Most moms report some immediate improvement after the procedure, but it can sometimes take up to a few weeks or months to resolve all of your breastfeeding challenges, depending on other confounding issues, such as mom’s milk supply or baby’s progress. Remember, your baby has been using his/her tongue and upper lip in this way since he/she was in utero, so it may take some time to ‘relearn’ how to use his/her tongue and upper lip effectively. Body work, such as craniosacral therapy and chiropractic, can help speed up this process as it can reset your baby’s nervous system, as well as relax the muscle tension that your baby may have developed while using compensating mechanisms.
Here are some additional online resources that have excellent information about tongue and lip ties. Stay tuned for our featured stories from moms whose breastfeeding challenges improved after having their babies’ tongue and lip ties revised. Better yet, sign up for our newsletter and have these articles delivered directly to your email inbox!
Websites that offer ways to see if your baby might be tongue tied:
Catherine Watson Genna: Is My Baby Tongue Tied?
Dr. James Ochi: Tongue Tie Survey
More researched-based articles about tongue and lip ties:
American Academy of Pediatrics Tongue Tie article
Dr. Kotlow: Tongue Tie Fact Sheet
The Leaky Boob: The Basics of Tongue and Lip Tie: Related Issues, Assessment, and Treatment
Boob Group episode: Tougue Ties and Lip Ties: Symptoms, Treatment, and Aftercare
If you would like to submit your personal story about breastfeeding a baby with a tongue or lip tie, please email it to robinkaplan@sdbfc.com
Did your baby have a tongue or lip tie?
How did this affect breastfeeding?
Baby Jaws - Breastfeeding a Teething (or Toothy!) Baby
Duh Nuh Duh Nuh………….Duh Nuh Duh Nuh. (come on, you know you just read that out loud).
You know they’re coming. You’ve heard all the severe warnings from well-intentioned friends and family. You’re scared of what’s to come, but know you’ve gone too far to turn back. Shark-infested waters, you ask? Noooooo - a breastfeeding baby who has grown TEETH!
Somewhere around 6-8 months (sometimes earlier, sometimes later), your baby’s first tooth will erupt. This is most likely an event you will celebrate, both because of the milestone that it is, but also because it may be a temporary break from the cranky, drooly, mouthy baby who replaced your own sweet one a couple of months back. There are lots of symptoms that point to teething, but the most common ones are: red and swollen gums, increased irritability and drooling, sleep disturbances, and low grade fevers. Your baby has most likely learned that chewing or gumming on items helps ease the pain and will try to cram everything within reach into his/her mouth. As that tooth begins to emerge, there may be some small worries creeping in on your excitement about this next stage. What will it be like to breastfeed a baby with teeth? Will my baby bite me? Some moms will find that they do start to feel the baby’s teeth while nursing - baby may scrape teeth across nipple when latching or delatching. And yes, sometimes the baby will bite.
Duh Nuh Duh Nuh………….Duh Nuh Duh Nuh. (come on, you know you just read that out loud).
You know they’re coming. You’ve heard all the severe warnings from well-intentioned friends and family. You’re scared of what’s to come, but know you’ve gone too far to turn back. Shark-infested waters, you ask? Noooooo - a breastfeeding baby who has grown TEETH!
Somewhere around 6-8 months (sometimes earlier, sometimes later), your baby’s first tooth will erupt. This is most likely an event you will celebrate, both because of the milestone that it is, but also because it may be a temporary break from the cranky, drooly, mouthy baby who replaced your own sweet one a couple of months back. There are lots of symptoms that point to teething, but the most common ones are: red and swollen gums, increased irritability and drooling, sleep disturbances, and low grade fevers. Your baby has most likely learned that chewing or gumming on items helps ease the pain and will try to cram everything within reach into his/her mouth. As that tooth begins to emerge, there may be some small worries creeping in on your excitement about this next stage. What will it be like to breastfeed a baby with teeth? Will my baby bite me? Some moms will find that they do start to feel the baby’s teeth while nursing - baby may scrape teeth across nipple when latching or delatching. And yes, sometimes the baby will bite.
Why did he bite me!?
Short answer is that it’s not because he doesn’t like you! New teeth bring a whole new sensation for baby. He may want to explore his world using his new teeth and will scrape and/or bite items that come into his mouth. Another reason that your baby may clamp down onto your nipple during a feeding is because of teething pain. As mentioned above, babies learn that biting and chewing on items may offer them some relief. If they are experiencing teething pain while breastfeeding, they may try to alleviate that pain by biting down. Or, your baby is finished with the feeding and wants to play!
Note: Sometimes when persistent nipple pain starts when the top teeth come in, it can be caused by an unresolved upper lip tie that is causing the baby’s top teeth to scrape against the nipple. Make sure your baby’s upper lip flanges out, like fish lips, to prevent this pain, or consider having his/her upper lip tie revised.
What should I do?!
Almost all moms will have the same reaction the first time their babies bite them while breastfeeding - some loud yelling and possibly a quick change of position! This is a completely normal and expected reaction, but you may notice the sudden sound and movement startles your baby. The best thing you can do is soothe your baby and resume the breastfeeding session. If your baby should bite you again, calmly remove the baby, give them a quiet vocal command (‘no’, ‘that hurts mommy’, etc) and temporarily end that feeding session. If your baby is still hungry, then offer the breast again to finish the breastfeeding session.
Also, some moms find it helpful to rub a cold, wet facecloth on baby's gums before latching to desensitize the teething pain before latching.
Because of the sucking mechanism babies use when breastfeeding, it is impossible for them to actually remove milk from the breast when they clamp down on the nipple, therefore biting may indicate baby isn’t hungry enough to feed. This is clear when a baby will bite towards the end of the feeding. One way to prevent this is to watch your baby while feeding, and when he/she starts to show signs that he/she is almost done (suck pattern will slow greatly, baby may come off often and smile and interact with you), calmly remove him/her from the breast and end the feeding session.
For almost all breastfeeding babies, this biting is a temporary phase. As they grow more accustomed to their new teeth and learn that biting means the breast is taken away, they will likely stop the behavior. If your nipples become cracked or sore because of any biting, we recommend applying organic coconut oil - it is soothing along with having antibacterial and antifungal properties.
Rest assured, the biting is normally a very fleeting behavior. Before long, the waters will once again be safe to enter.
Common Concerns While Breastfeeding - What is That White (and painful!) Spot on My Nipple?
Welcome back to our blog series…. Common Concerns While Breastfeeding. These aren’t the complicated, ‘come-to-my-house-immediately’ phone calls we receive. Rather, these are the questions that come from clients and friends in the middle of the night, by text or by email, that don’t necessarily warrant a lactation consultation. They can often be easily resolved with a few simple tricks. So, we would like to share those tricks with you!
Many moms know the pain associated with a shallow latch during the early days, but have you ever had nipple pain suddenly begin after weeks or months of pain-free breastfeeding? After checking nipples for signs of a poor latch, you notice a white spot on the nipple in question - you pick at it for a few seconds, but it still remains. What is it? What caused it? What can you do to resolve it and get back to pain-free breastfeeding? This is what’s called a “milk blister” or “milk bleb” and is not cause for great concern, but it can be an uncomfortable and unwelcome guest!
Welcome back to our blog series…. Common Concerns While Breastfeeding. These aren’t the complicated, ‘come-to-my-house-immediately’ phone calls we receive. Rather, these are the questions that come from clients and friends in the middle of the night, by text or by email, that don’t necessarily warrant a lactation consultation. They can often be easily resolved with a few simple tricks. So, we would like to share those tricks with you!
Many moms know the pain associated with a shallow latch during the early days, but have you ever had nipple pain suddenly begin after weeks or months of pain-free breastfeeding? After checking nipples for signs of a poor latch, you notice a white spot on the nipple in question - you pick at it for a few seconds, but it still remains. What is it? What caused it? What can you do to resolve it and get back to pain-free breastfeeding? This is what’s called a “milk blister” or “milk bleb” and is not cause for great concern, but it can be an uncomfortable and unwelcome guest!
What is a milk blister?
A milk blister is a small white or yellow spot on your nipple - it is normally blocking a milk duct, hence sometimes the pain associated with it is felt both at the tip of the nipple as well as radiating out into the breast. It can’t easily be wiped away or removed. It may sometimes be associated with a plugged duct. It is perfectly safe to continue to breastfeed while you have one.
What causes a milk blister?
There are two causes for what we call a milk blister. One is that a bit of skin has grown over an open milk duct, blocking it and creating a blister. The other is the build up of fatty milk at the site of the milk duct, and the calcification of this fatty milk, which then blocks milk from flowing from this duct. The things that can increase risk for a milk blister are:
A recent plugged duct
Nipple is pinched often while baby is breastfeeding
Oversupply
Unusual pressure from a bra or sleeping position
How can I get rid of the milk blister?
Place some organic coconut oil on a cotton ball and place it on your nipple, inside your bra, in between feedings for a few days. This will help break down the calcification at the tip of the nipple, as well as fight off any bacteria or yeast.
Soak your nipple/breast in a saline bath of warm water several times a day. According to Kellymom.com, add 2 tsp of epsom salt to 1 cup hot water. Allow the salt to dissolve and soak your affected breasts prior to feeding. Then place a hot, wet facecloth over your breast right after the saline bath and right before breastfeeding/pumping. This should help to soften the nipple and help the blister release while baby is feeding or while pumping.
Apply moist heat to nipple prior to feeding
Try to remove the skin prior to feeding - rub with a warm washcloth
If all else fails, you can also ask your healthcare provider to use a sterile needle to open the blister. After this procedure, follow up with organic coconut oil to keep the area moist and allow it to heal.
What if I keep getting milk blisters?
Consider seeking help from a Lactation Consultant to try to resolve the underlying cause of the recurring blisters.
Be sure your bras provide soft but strong support - avoid ones with underwire that may cause plugged ducts.
Consider reducing the amount of saturated fat in your diet.
Consider taking sunflower lecithin, 1200mg, 4 times a day, to keep milk ducts ‘slippery’ thereby preventing recurring plugged ducts and milk blisters.
What Every Mom Should Know About Breastfeeding During the Early Weeks
How much breast milk does my baby need per feeding?
What is common nursing behavior for a newborn?
How will I know that my baby is getting enough?
As a new mom, these are common questions that you may ask your pediatrician, midwife, postpartum nurse, family, and friends and GUESS WHAT..... they may all have a different answer!
How much breast milk does my baby need per feeding?
What is common nursing behavior for a newborn?
How will I know that my baby is getting enough?
As a new mom, these are common questions that you may ask your pediatrician, midwife, postpartum nurse, family, and friends and GUESS WHAT..... they may all have a different answer!
How complicated is that?
Sometimes you may feel like there are ‘too many cooks in the kitchen’ and that all of the advice you receive contradicts what you just heard from someone else 5 minutes ago.
Talk about frustrating!
Well, one of our goals at the San Diego Breastfeeding Center is to make breastfeeding as seamless and uncomplicated as possible. We want to empower moms with knowledge and confidence to get breastfeeding off to a great start!
After listening to local moms express discontent about hearing contradictory breastfeeding information, we decided to do something about it. First, we canvased our local breastfeeding mamas and asked, “What information do you wish you would have known about breastfeeding during those early weeks?” Then we hired one of those awesome mamas, Elisa Suter, of Paper Doll Design Studios, to design a brochure that shares our top tips that every mom (and pediatrician) should know about breastfeeding during the early weeks.
Here is the final product! Isn’t it beautiful? We hope that this brochure provides the clear, consistent, evidence-based breastfeeding information our mamas are looking for.
If you live in San Diego and would like us to deliver these brochures to your pediatrician's office, please email us at robinkaplan@sdbfc.com.
If you live outside of San Diego and would like to order the Adobe file to personalize this brochure for YOUR local pediatricians and clients, please email us at robinkaplan@sdbfc.com
Keeping Up Your Milk Supply During the Holiday Season
Since Winter Break has descended onto our homes, Ashley and I are taking the next few weeks off from blogging to spend some quality time with our families. However, that doesn't mean that you'll be left without our breastfeeding support until the new year! We have over 300 articles on the San Diego Breastfeeding Center blog, which means there is no reason for you to google 'sore nipples' at 3:30am. Just check out our extensive article list and you will be well on your way!
Here are some of our favorite tips for keeping up your milk supply during the holidays
Since Winter Break has descended onto our homes, Ashley and I are taking the next few weeks off from blogging to spend some quality time with our families. However, that doesn't mean that you'll be left without our breastfeeding support until the new year! We have over 300 articles on the San Diego Breastfeeding Center blog, which means there is no reason for you to google 'sore nipples' at 3:30am. Just check out our extensive article list and you will be well on your way!
Here are some of our favorite tips for keeping up your milk supply during the holidays
- Holiday recipes often include herbs that can affect supply. Don't eat too much sage or mint - these are herbs used to temper down or dry up a mom's milk supply. One mint cookie won't do it, but be aware of the amounts you are consuming.
- Continue to breastfeed or pump at regular intervals. It's very easy to skip feedings and/or pumping sessions with all of the holiday festivities, which can lead to plugged ducts and mastitis. Yuck! Try to stick to your regular breastfeeding/pumping schedule to prevent your breasts from getting overly full and uncomfortable.
- Traveling during the holidays, expecially with a baby or toddler, can really wear your body down. To keep up your milk supply, stay hydrated, bring tons of nourishing snacks for the trip, and do you best to get good sleep. Plus, follow your child's lead and squeeze in a nap or two throughout the trip. Your immune system will definitely thank you for it!
- Find your comfort level with breastfeeding around family members. Enlist your partner as your cheerleader and advocate so that you can feel comfortable breastfeeding your baby in all holiday situations. If you feel timid around certain family members and friends, invest in a breastfeeding cover, like this one from Bebe Au Lait, so you don't have to leave the room everytime your baby is hungry. It's also a good idea to practice at home in front of a mirror, you'll see how very little of your breast is actually exposed and this may help you to feel more comfortable.
- If you start feeling under the weather, stick with herbs and over-the-counter medications that don't dry up your mucus membranes, as they may dry up your milk supply as well. Herbs that support your immune system, that are safe to take while breastfeeding, are echinacea and vitamin C. If you feel like you are coming down with a cold, you can take homeopathic oscillococcinum and yin chiao to build your immune system and speed up your recovery. For over the counter medications recommendations, listen to our Boob Group podcast with Dr. Frank Nice, Breastfeeding and Medication. You can also contact your local lactation consultant and ask her to look up a particular medication to see if it is safe to take while breastfeeding.
Lastly, here are some of our most popular breastfeeding articles to help you through the holiday season:
Advice for the Newly Breastfeeding Mama's Partner
Help A Mama Out; Ways Partners Can Bond with Baby Besides the Bottle
Help A Mama Out: Overcoming Nursing in Public Anxiety
Common Concerns While Breastfeeding: Sore Nipple Therapy for the Breastfeeding Mom
Common Concerns While Breastfeeding: Yikes! Why are my Nipples Burning?
Common Concerns - Do I Have Mastitis?
We wish you a beautiful, peaceful holiday season and look forward to sharing more judgment-free breastfeeding resources with you in the new year!
Warmly,
Robin and Ashley
Breastfeeding My Type 1 Diabetic Daughter
Almost 2 years ago, a dear friend of mine found out that her 19 month old daughter had type 1 diabetes and was fighting for her life. Here's Theresa's triumphant story of how she was able to preserve her breastfeeding relationship while healing her daughter.
_____
About a month ago a friend alerted me to a Facebook post that brought a wave of memories flooding over me from a day that changed my life forever as a parent. A day that I will never forget, even though I wish I could. It was literally the worst day of my life, but one that I will always be grateful for because it was the day my daughter’s life was saved.
Almost 2 years ago, a dear friend of mine found out that her 19 month old daughter had type 1 diabetes and was fighting for her life. Here's Theresa's triumphant story of how she was able to preserve her breastfeeding relationship while healing her daughter.
_____
About a month ago a friend alerted me to a Facebook post that brought a wave of memories flooding over me from a day that changed my life forever as a parent. A day that I will never forget, even though I wish I could. It was literally the worst day of my life, but one that I will always be grateful for because it was the day my daughter’s life was saved.
The Facebook post was from a worried mom whose child was hospitalized after being diagnosed with type 1, “juvenile,” diabetes that very day. The mama was breastfeeding and was terrified not only for her child's life, but that she would lose the best way she knew to feed and comfort her baby. A little over a year and a half ago I was in her shoes. At 19 months old, we were told that our daughter had type 1 diabetes, was in diabetic shock, and needed to be rushed to the emergency room. She came very close to losing her life and was in critical care for a week at a children’s hospital.
While she was at her sickest (almost admitted to the ICU), she was not allowed to nurse. For as comforting as breastfeeding can be, not being able to do it during a time of crisis was torture. My daughter was barely conscious, was in pain and terrified while she was awake, and I could not even hold her because she wanted to nurse. I hope no other mama has to experience the excruciating helplessness you feel in a situation like that. Our children's hospital has no lactation consultants and, by the time they could find a pump for me, we had already skipped about 7 or 8 feedings. I was scared to death and in physical pain myself.
When we were finally given the okay for her to eat, I had to fight tooth and nail to be able to breastfeed her. The doctors finally consented to her having breast milk, but because she was not a tiny baby, the doctors did not think it was important. They told me that she absolutely had to drink from a cup or bottle. (I had a manual pump at home and did not respond well to it at all. I could not imagine how difficult it would be to have to exclusively pump.) I begged them to let me nurse her. It was my milk after all, whether it came from a pump and was poured directly into a cup or came straight from my breast. No mother should ever have to beg to be able to feed their baby. It took hearing our daughter scream and sob hysterically for the doctor to finally take pity on us and let me breast feed her. As I held my tiny girl in my arms, it was the first time I began to feel like there was a possibility that she would be okay. Still, we were encouraged to not let her nurse after that.
Eventually, we were able to meet with the hospital's diabetes dietician who helped me calculate the average amount of milk I produced per feeding. We looked at the amount of milk I was able to express with a pump then, by using the general amount of carbohydrates contained in breast milk, we were able to determine a rough estimate for carbohydrates per feeding. Together we came up with a plan to space out her feedings as much as possible to keep her blood glucose stable (after each meal and to go to sleep). The dietician was a lifesaver and a champion for us! She spoke with our doctor on our behalf and convinced him that including breastfeeding as part of our daughter's nutrition was in her best interest. The doctor has since become supportive.
Continuing breastfeeding brought my daughter so much comfort in the months of learning to live with daily multiple injections and painful finger prick blood tests. It was something normal and peaceful for both of us during a stressful time of adjustment. It supported her overall health. It was a perfect source of nutrition for her combined with solids and was amazing for bringing her blood glucose back up to a safe level if she began to drop low at night (we do use a fast acting sugar, like juice, instead if she is below a safe threshold). I am so thankful that we were able to continue our nursing relationship until she was 32 months old.
Type 1 diabetes (T1D) is a life-threatening, autoimmune disease in which a person’s body attacks their pancreas, causing it to stop producing insulin, a hormone needed to properly process carbohydrates in the food we eat. People with type 1 diabetes check their blood glucose levels every few hours and must inject insulin several times every day or continuously infuse with insulin through a pump. There is no known cause of type 1 diabetes and, at this time, no cure. It will never go into remission and cannot be reversed. As a mom, you can't help but wonder if you caused it somehow but, it just isn't possible that you did. It is not connected to poor diet or lack of exercise. Our daughter never has had a drop of formula, never had sugar other than that naturally occurring in fruit, never drank juice prior to needing it to treat hypoglycemia, and eats primarily homegrown, organic solid food.
Not many people think that a baby or toddler can develop type 1 diabetes, however it is definitely possible. Not all doctors think of it either and it is commonly misdiagnosed as the flu, with deadly results. It is very important to know the possible warning signs. I would recommend all moms be aware of any major changes in nursing. A sudden onset of increased nursing (past the length of time a growth spurt or teething would account for) along with much more frequent wet diapers can be a signal of diabetes. Diaper rash (especially without a history of it) and yeast infections can be symptoms of high blood glucose. Also, consider vitamin D supplements if a blood test returns low for vitamin D levels and investigate further if the test results are extremely low. The researchers think there may be a link between low vitamin D and diabetes, however they don't know if it is a cause of diabetes or a symptom of it. Our daughter had increased nursing and wet diapers, weight loss and developed labored breathing. Thankfully our pediatrician picked up on the problem and took action immediately.
Warning signs of type 1 diabetes can include:
• Extreme thirst
• Frequent urination
• Drowsiness, lethargy
• Sudden vision changes
• Increased appetite
• Sudden weight loss
• Fruity, sweet, or wine-like odor on breath
• Nausea or vomiting
• Heavy, labored breathing
• Stupor, unconsciousness
• Sugar in urine
Most importantly, if you feel that something is wrong, go with your gut and keep asking until you find answers! A quick finger prick test to check the blood glucose level can rule out diabetes. For this test, a small drop of blood from the tip of the finger is sampled. Results are often immediate. A simple urine test can also check for abnormalities. Undiagnosed and untreated T1D can become deadly very quickly.
If you have a little one diagnosed with diabetes, ask to speak to the nutritionist about continuing to incorporate breastfeeding into their nutritional plan. By pumping once and measuring the amount expressed or by weighing the baby before and after feeding they can help you determine the general amount of milk and therefore carbohydrates they receive at the breast with each feed. (Because it is an estimated number and not exact, they can often account for the difference in the allotted carbohydrate plan.)
Also, there are amazing support resources available for small children with T1D! Facebook groups like “Diapers & Diabetes” and organizations like JDRF offer support for families, education, a place for children to feel encouraged and like any other child, and help navigate the uncertain and ever-changing waters that are type 1 diabetes. Additionally, JDRF funds research and is constantly striving to improve life for type 1 diabetics. Most importantly, they are fighting for a cure for type 1 diabetes.
*** Please note that these are just our experiences. I'm not giving medical advice and don't claim to be an expert on diabetes--I'm just a breastfeeding mom doing everything she can to keep her daughter healthy! Seeing her grow and thrive, and watching her play momma and nurse her baby dolls, I think I might be doing an okay job.
If you want to learn more about type 1 diabetes, www.jdrf.org is a wonderful resource. For a glimpse into our life with it or to help fund a cure, please visit:
http://www2.jdrf.org/site/TR/Walk-CA/Chapter-SanDiego4053?px=2922459&pg=personal&fr_id=2382
or watch our story at: https://www.youtube.com/watch?v=2Fc6r8HEnn0
My Village of Breastfeeding Support
Over the next few weeks we will be sharing stories of triumphant breastfeeding mamas and their biggest supporters who helped them reach their personal breastfeeding goals. If you would like to share your breastfeeding story and thank your biggest breastfeeding cheerleaders, check out the details in our recent blog article.
_____
Here is Stephanie's story.
It has truly taken a village to help me be successful in nursing both of my babies! I knew I wanted to breastfeed, but, after the birth of my first son, my passion and commitment to it were a surprise to even me. I was also caught extremely off-guard by the difficulties both of my boys encountered as we began our breastfeeding journeys together. Tongue ties, lip ties, low weight gain, low supply, poor latch, pain/cracking/bleeding, overactive letdown, and more were all hurdles we had to cross. There is absolutely NO way I could have made it to 13 months formula-free with my first son and still going strong and formula-free at 6 months with my second without these amazing people.
Over the next few weeks we will be sharing stories of triumphant breastfeeding mamas and their biggest supporters who helped them reach their personal breastfeeding goals. If you would like to share your breastfeeding story and thank your biggest breastfeeding cheerleaders, check out the details in our recent blog article.
_____
Here is Stephanie's story.
It has truly taken a village to help me be successful in nursing both of my babies! I knew I wanted to breastfeed, but, after the birth of my first son, my passion and commitment to it were a surprise to even me. I was also caught extremely off-guard by the difficulties both of my boys encountered as we began our breastfeeding journeys together. Tongue ties, lip ties, low weight gain, low supply, poor latch, pain/cracking/bleeding, overactive letdown, and more were all hurdles we had to cross. There is absolutely NO way I could have made it to 13 months formula-free with my first son and still going strong and formula-free at 6 months with my second without these amazing people.
My husband! My passion and commitment to breastfeed my babies surprised him also, but he never questioned it and stood by me no matter what decisions I made! He became just as committed and passionate about it, knowing it was the best thing we could do for our boys. He came to appointments, helped get the baby latched on time after time, stood up for me when others questioned why I didn’t just quit, and let me cry when it all just became too much! He has truly been my rock through all of this, and I can sense his gratitude for the sacrifices I have made to give our boys this amazing gift!
My Lactation Consultants! Four different lactation consultants have come alongside my babies and me in our journey together. Every single one of them encouraged me that I could do it when the hurdles seemed insurmountable. They provided a listening, sympathetic ear when I just needed to vent or cry or talk it out. They provided help, advice, referrals, and life-changing solutions that kept us going!
My tribe of other breastfeeding Mamas! Friends I have known since childhood, friends I’ve made in recent years, and people I met through the breastfeeding process made it all possible - others who had or were experiencing some of the same challenges, some who didn’t have trouble but believed just as passionately in the benefits of breastfeeding, some who visited, some who called, and one who even created an on-line community to connect us all! There were many people in my life who didn’t understand why I didn’t give up when they saw the emotional and physical toll it was taking on me, but these other Mamas got it! They knew why I couldn’t quit, why no challenge was too big!
My virtual breastfeeding community! Although I will never meet most of these women in person, the support, advice, commiseration, and encouragement they have provided have truly been critical! To be able to jump online in the middle of the night when it just seemed like I couldn’t do it and have others on there to tell me that, yes, I could do it got me through many rough moments! They have calmed nerves, answered questions, given virtual hugs, and just been an amazing support system!
My babies! Even from the very start and even in the face of all of our challenges, my babies have always loved nursing! They didn’t quit so there was no way I could!
Breastfeeding in the Operating Room
Over the next few weeks we will be sharing stories of triumphant breastfeeding mamas and their biggest supporters who helped them reach their personal breastfeeding goals.
_____
This story is from Dawn.
I have to thank my hospital TEAM for my breastfeeding success!
When I gave birth to my son 5+ years ago, it wasn’t what any first time mom would like to experience. I was having problems with maintaining my blood pressure and when my little boys’ heart rate dropped too low, I was rushed into an emergency c-section. It was an extremely frightening process that didn’t even enter my mind as a possibility. The months that followed were hard. We struggled at finding a proper latch and feeding became such a difficult task, I dreaded it.
It never occurred to me that our difficulties at latching could have been because of the birth experience .
Over the next few weeks we will be sharing stories of triumphant breastfeeding mamas and their biggest supporters who helped them reach their personal breastfeeding goals.
_____
This story is from Dawn.
I have to thank my hospital TEAM for my breastfeeding success!
When I gave birth to my son 5+ years ago, it wasn’t what any first time mom would like to experience. I was having problems with maintaining my blood pressure and when my little boys’ heart rate dropped too low, I was rushed into an emergency c-section. It was an extremely frightening process that didn’t even enter my mind as a possibility. The months that followed were hard. We struggled at finding a proper latch and feeding became such a difficult task, I dreaded it.
It never occurred to me that our difficulties at latching could have been because of the birth experience.
In early 2012 we received good news, we were expecting! I did my best to set everything up for a different birthing experience. I searched out a CDC accredited Baby Friendly Hospital in my area, researched VBAC’s and educated myself on the benefits of skin-to-skin. It wasn’t until closer to my due date that I was informed I couldn’t have a VBAC. No hospital would even consider me as a potential VBAC candidate because of my small heart issue as well as my age. After fighting and pleading, I had to acknowledge that I had no other option, but another C-section.
I may have lost that battle, but I was going to do everything in my power to have skin-to-skin with my little girl. I was aware of the evidence-based research on the benefits of skin-to-skin and its success rate with c-section births. I talked to my pediatrician about this and he agreed. (I since found out that it is the pediatrician who is in charge in the OR!) I wrote my birth plan with the intentions of doing skin-to-skin immediately after the c-section unless there was a medical reason not to.
Alas, I wasn’t able to make it all the way to my scheduled c-section date. This time I was low on amino fluids and baby’s lack of movement put me into the hospital at 36 weeks. With concern, my OB and the pediatrician, agreed, that under supervision, they would monitor me and try to get us to the 37th week and do the c-section.
Now, prior to this, we made sure to talk with all the right people about our wishes for skin-to-skin. Everyone was on board: our OB, the hospital’s labor and delivery nurses, and staff. In fact, the hospital staff has been championing the change in procedures to allow skin-to-skin in the OR without success.
The day of my C-section, my regular pediatrician was out of town and his standing replacement wasn’t comfortable at all. I had to conveince the standing pediatrician that this was in my and my baby's best interest. The hospital's Head Labor & Delivery nurse helped us get to a compromise! She is my angel! She proposed that if everything looked good my little girl would be immediately placed on my chest, without ANY other intrusion.... meaning the vernix would be wiped off her while she was on my chest and she would be weighted and measured later.
When the hour came for us to have the c-section more drama around skin-to-skin unfolded, this time all the way up to the director of the Family Birth Center. The director of the Family Birth Center was completely opposed to it and tried talking my OB out of it. We were lucky we had enough support and commitment from the labor and delivery nurses and my OB to move forward. We finally got our wish!
I have to admit, because she was coming 3 weeks early, I wasn’t sure we would even get the option of skin-to-skin, but our little girl emerged perfectly! She was screaming and quickly confirmed in perfect health!
When she was placed on my chest and covered with a warming blanket, I was in awe. This little 6 pound bundle was just perfect. After a little while, she actually scooted and rooted for my breasts and eventually latched and nursed! I just didn’t think I would get that experience since she was early. The remembrance still makes me cry. It was such an amazing experience. I was so happy I had the team in my corner and the hospital went forward with my wishes.
When I was first told I would have to have another cesarean, I felt completely out of control and very disappointed. Creating a birth plan around my c-section allowed me to take a bit of control back and talking with all parties that come with a c-section allowed me the skin-to-skin connection that was deeply important to me.
It has been over a year since Beth was born. We are still nursing strong and have a connection that I attribute to the wonderful team that helped me get skin-to-skin in the OR!
Side note: I have since heard that they have allowed other moms the same experience! The hospital team not only helped me, but also have persevered in getting policy “changed” at the hospital!
Dawn Alva
Comebacks for ‘Why Are You Still Breastfeeding?’
Any woman who has ever had a breastfeeding challenge or has breastfed longer than than someone else deems ‘normal’ has been asked this question at one time or another.
“Why are you still breastfeeding?”
Sometimes this question is passive aggressive with undertones of “I can’t believe you have breastfed your baby for THIS long.” Other times it comes from a place of love meaning “You seem like you are in pain... are you sure you still want to try this?”
Regardless, if you are anything like me, the snappy comeback or educated response that I SO desired to say only comes after the situation is long gone and I am kicking myself for not defending myself and my choice to breastfeed the way I wanted to.
Any woman who has ever had a breastfeeding challenge or has breastfed longer than than someone else deems ‘normal’ has been asked this question at one time or another.
“Why are you still breastfeeding?”
Sometimes this question is passive aggressive with undertones of “I can’t believe you have breastfed your baby for THIS long.” Other times it comes from a place of love meaning “You seem like you are in pain... are you sure you still want to try this?”
Regardless, if you are anything like me, the snappy comeback or educated response that I SO desired to say only comes after the situation is long gone and I am kicking myself for not defending myself and my choice to breastfeed the way I wanted to.
Well, ladies... look no further!
Here are some handy, snappy (evidence-based) comebacks that you can tuck away in your back pocket, only to whip out at the most appropriate times, pun intended! (P.S. These comebacks also work if someone asks why you are STILL exclusively pumping!)
Top 10 Comebacks to Answer the Question: Why Are You Still Breastfeeding?
1. “It’s the perfect food for my child. 24 hours a day, 7 days a week!”
- Babies can digest human milk more easily than the milk of other animals, probably because human milk contains an enzyme that aids in this process.
- Breast milk forms softer curds in the infant's stomach than cow's milk (the basis for most formulas) and is more quickly assimilated into the body system.
- While it contains less protein than does cow's milk, virtually all the protein in breast milk is available to the baby. By contrast, about half the protein in cow's milk passes through the baby's body as a waste product.
- Similarly, iron and zinc are absorbed better by breastfed babies.
2. “Breastmilk doesn’t lose it’s nutritional value. Can you say that about the food YOU eat?”
- Even at a year, breastmilk continues to pack a powerful punch for nutritional value.
- In the second year (12-23 months), 448 mL of breastmilk provides:29% of energy requirements
- 43% of protein requirements
- 36% of calcium requirements
- 75% of vitamin A requirements
- 76% of folate requirements
- 94% of vitamin B12 requirements
- 60% of vitamin C requirements
Dewey KG. Nutrition, Growth, and Complementary Feeding of the Breastfed Infant. Pediatric Clinics of North American. February 2001;48(1), from Kellymom.com Breastfeeding Past Infancy Fact Sheet
3. “Breastmilk protects against disease for my baby. Don’t you want my (our) baby to be healthy?”
- Because the mother makes antibodies only to pathogens in her environment, the baby receives the protection it most needs-against the infectious agents it is most likely to encounter in the first weeks of life.
- Here are a few ways that breastmilk helps make a healthy baby:
- Breastfed babies also have less diarrhea and fewer gastrointestinal infections than babies who are artificially fed.
- Six months or more of exclusive breastfeeding reduces risk of food allergies.
- Breastmilk decreases a child’s risk of Crohn's disease and ulcerative colitis in adulthood.
- Breastfed babies have lower risk for developing recurrent wheezing when they are older (age 6 or more) – asthma
- They have less reflux
- They have less eczema
- Breastfeeding protects baby against respiratory infections
- Women who were formula-fed as infants have higher rates of breast cancer as adults. For both premenopausal and postmenopausal breast cancer, women who were breastfed as children, even if only for a short time, had a 25% lower risk of developing breast cancer than women who were exclusively formula-fed as infants.
4. “There are incredible health benefits for my breastfed baby. Do you really think it’s wise to limit my baby’s intellectual and physical potential?”
- Breastfed children have higher IQ
- Breastfeeding reduces a baby’s risk of SIDS by 50%
- Breastfeeding protects baby against vision defects. Breast milk is generally the main, if not the only source, of vitamin A during a child's first 24 months of life (or for the duration of breastfeeding).
- Suckling at the breast is good for a baby's tooth and jaw development, as the constant pulling at the jaw muscles promotes a well-formed jaw and healthy teeth.
5. “Breastfeeding improves my overall health. Who’s going to cook all of the meals and take care of the home if I’m not healthy? (I know...super snarky!)”
- Breastfeeding decreases mom’s risk of postpartum hemorrhaging as it stimulates contractions to shrink he uterus back to pre-pregnancy size.
- Breastfeeding reduces mom’s risk of osteoporosis
- Breastfeeding reduces mom’s risk of anemia, as breastfeeding postpones the return of menstruation for many women.
- Breastfeeding reduces mom’s risk of breast cancer. Women who breastfeed reduce their risk of developing breast cancer by as much as 25 percent. The reduction in cancer risk comes in proportion to the cumulative lifetime duration of breastfeeding. That is, the more months or years a mother breastfeeds, the lower her risk of breast cancer.
- Breastfeeding reduces the risk of uterine and ovarian cancer.
6. “Breastfeeding promotes mother/infant bonding and emotional well-being.”
- Babies feed for about 45 minutes per time in the first few months. This is nature’s way of making moms sit down and relax and promote her postpartum healing.
- Breast milk actually contains chemicals that suppress pain (endorphins). This is the perfect remedy for a child who accidentally hurts himself and is in need of some pain relief and comfort. It's like having a boo-boo-healing superpower!
- Babies can also feel the warmth of mom's skin, take in her scent and hear her heart beating. This helps to neurologically center thebaby after birth and help him/her adjust to the outside world.
- Breastfeeding also decreases a mother’s risk for postpartum depression.
7. “Breastfeeding can promote a positive relationship between mom and a supportive partner.”
- Partner support is crucial during breastfeeding, especially when there are challenges along the way.
- In the beginning, when baby is pretty much just eating and sleeping, mom and her partner can spend this time together, hanging out while the baby is feeding, getting to know one another as parents, not just partners.
- This is a great time to reconnect with your partner as the both of you get to know your baby, as this is a new time for your family.
- You are also a team during this time. Partners can make sure that all visitors offer positive breastfeeding comments, especially when breastfeeding is a challenge. No sabotaging comments allowed!
8. “Breastfeeding is definitely more convenient and less expensive than formula. I thought we were on a tight budget!”
- Breast milk, in any supply, is free. Ready-made formulas can cost families $800 to $1800 per child, annually.
- Nipples, bottles, bottle brushes and bottle bag inserts are additional costs, as well.
- Breastfed babies are ill less often, meaning that their parents miss fewer days at work and spend less on prescriptions, doctor's visits, and hospital stays.
9. “Breastfeeding, just like parenting, has bumps along the road and I won’t quit on my worst day.”
- As all thing that have to do with parenting, what works some days, doesn’t work on others and most things don’t go smoothly as planned.
- Your baby is born with a personality and a style that requires becoming familiar with and understanding.
- What works for some babies and children may not work for yours, so seek support anywhere you can find it: friends, family, lactation consultants, websites, Facebook groups, physicians, etc.
- Don’t quit on your worst day. Let 24 hours pass to gain some perspective and reach out for help during that time.
- Have an IBCLC evaluate your situation and provide a plan for overcoming your challenge.
10. “I promise you that my child won’t breastfeed until his high school graduation, but if he did, he’d probably be the smartest, healthiest graduate there!”
- Ok, maybe that’s a little too sassy, but you get the point. It is your choice to breastfeed for as long as mutually beneficial for you and your child. Every drop of breastmilk your child gets is liquid gold and you are a superstar for producing that for him/her! So stay strong, mama, and know that your ‘breast friends’ have your back! Happy nursing!